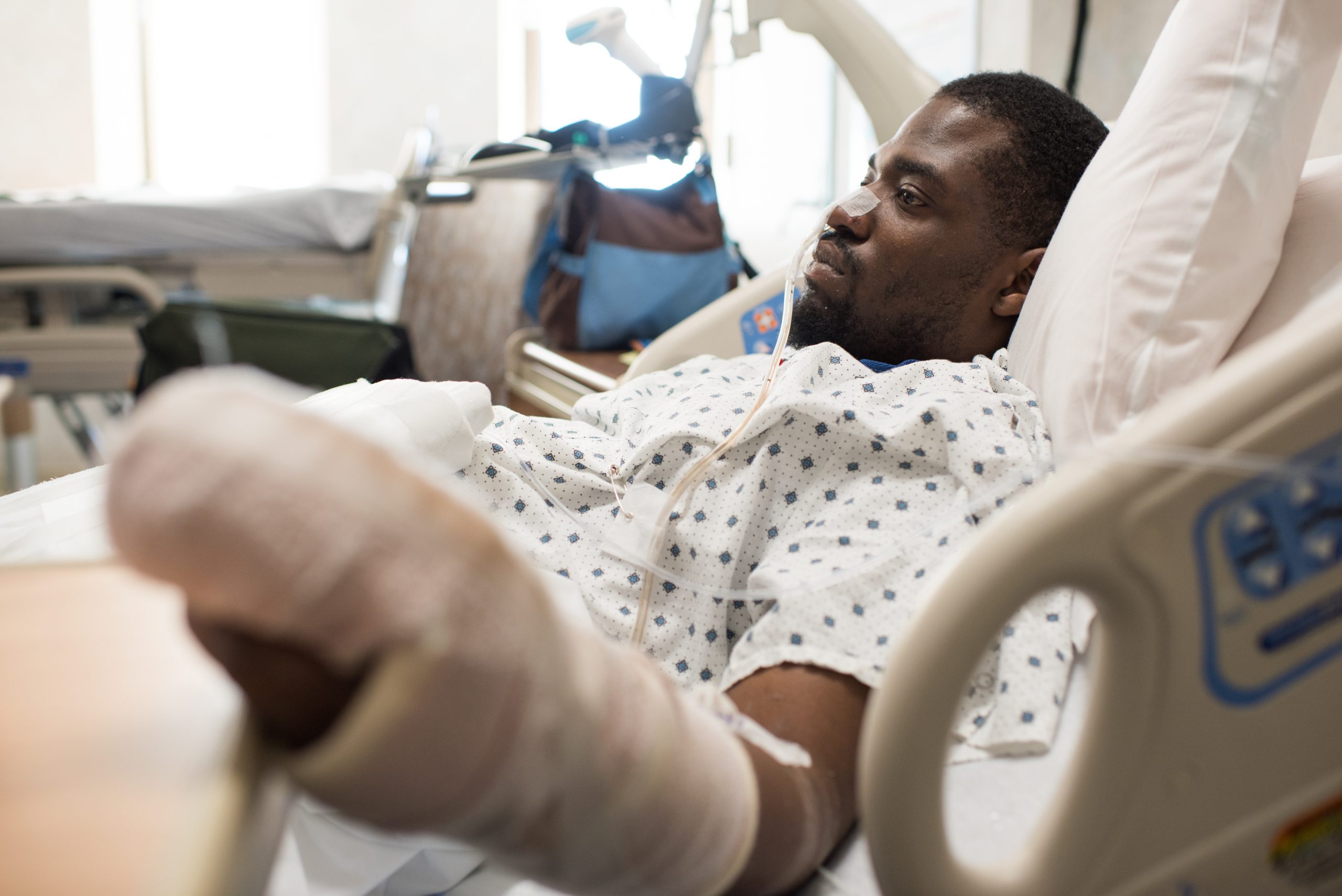
The first time Matthew Roberts was shot, a single bullet grazed the top of his shoulder. He remembers it as a warm day in 2015; he’d gone to see his girlfriend fight someone on the street in Cleveland, where he lives. A guy pointed a gun at him and pulled the trigger. “It went through,” he says, and out the other side. “Not really much pain.” Roberts didn’t bother going to the emergency room. Back at home, he says his girlfriend dipped a cotton swab in alcohol and peroxide, cleaned his wound, and covered it with a bandage.
The second time Roberts was shot came a few months later. He’d been waiting for a girl at a bus stop when he says a man pressed a gun to his back — Roberts guesses the guy was trying to steal his phone. This time, a trip to the hospital was not optional. Doctors removed the bullet and kept him in recovery for a few weeks. Then, they sent him home.
The third bullet found Roberts last November. He was hit as he stood outside a bar late one night. Doctors patched him up, again. Again, they released him back into the same streets where he had been shot before.
The fourth time Roberts was shot would be different. “Every other bullet, I was able to walk away from,” he says. Not this time. One evening in early December, a car pulled up in front of his house and a passenger fired — the latest strike in a long-standing beef, Roberts thinks. The bullet tore through his collar-bone and lung before lodging in his spine.
Roberts is 25 years old. He is now paralyzed. In the past months he’s been transferred between three different rehabilitation facilities. When he returned home earlier this month, it was in a wheelchair.

Americans suffer more than 80,000 nonfatal firearm injuries a year, three quarters of them from assault. A significant number of those shot, like Matthew Roberts, will sustain another gunshot wound or other violent injury in the future. In Cleveland, one study shows as many as one in three victims of gunshot or stab wounds return to the hospital for a separate traumatic injury. Other research has shown that shooting victims are at heightened risk of going on to commit violent crime themselves.
At the hospital, “trauma” is usually shorthand for the patient’s physical injury, which modern medicine is increasingly adept at treating. But there is also the trauma that transcends stitchable wounds. It’s this invisible damage — to a victim’s emotional or social life, or employment prospects, or stable housing — that leaves traumatically injured patients at elevated risk for getting seriously hurt again. Federal assistance meant to address those often unseen needs comes largely from a fund established by the Victims of Crime Act (VOCA), which each year hands money over to states to distribute. Drawing from federal criminal penalties and fines, the fund goes to a mix of direct financial compensation and support for services like crisis intervention, counseling, and emergency shelter.
But organizations that provide help to crime victims often don’t manage to reach people like Roberts. Victim advocates and experts on the law say that in the 32 years since VOCA was passed, much of the money earmarked for services has gone to well-established organizations that work with domestic violence and sexual assault victims, with less of it flowing to survivors of street violence, who historically have lacked institutionalized support of their own.

According to national statistics from the Office for Victims of Crime, which administers the funds, 48 percent of the people served through VOCA in 2015 were domestic violence victims, while just 7 percent were victims of assault, the category that survivors of street shootings would typically fall into.
Organizations advocating for gunshot victims now have an unprecedented opportunity to expand the support they can give. Thanks to a build-up of VOCA funds that Congress moved two years ago to begin spending down, states have seen their federal money for victims assistance increase dramatically — coinciding with rising homicide rates in major cities around the country. Nationally, the VOCA cap rose from $745 million to $2.36 billion in 2015. Ohio’s funds alone quadrupled to nearly $70 million, up from $16 million the year before.
The state’s Republican attorney general, Mike DeWine, decided to try something new with that money. After a year of planning, his office made Ohio the second state in the nation to unveil what’s known as a trauma recovery network, modeled after a seminal effort in California. Though the initiative comes from the state’s criminal justice system, the task of implementing it will fall to health care providers, social workers, and mental health professionals.
The five Ohio hospitals in the network’s initial $2.6 million phase are partnering with local service providers to offer trauma screening and crisis intervention that begins when victims of violent crime arrive in the emergency room. As patients heal and return to their community, social workers and trauma specialists will link them with a variety of services, including short-term safe housing, legal advocacy, referrals to substance abuse treatment, mental health counseling, and essentials like food and clothing. It’s an approach guided by the mantra that “hurt people hurt people” — the idea that both physical violent injury and psychological trauma can fuel future violence.
“A hospital’s primary focus should always be a patient’s physical well-being, but victims of violent crime suffer in other ways,” DeWine said when his office unveiled the new network in late January. “This program will ensure that victims will not have to seek out support on their own, because help will immediately be brought to them.”
To have a state’s top law enforcement official devoting dollars to a holistic public health program marks a “profound” shift, says Lenore Anderson, president of the Alliance for Safety and Justice. Her organization works to reduce incarceration and racial disparity nationwide, and brought the notion of a trauma recovery network to DeWine’s staff. “You have people in the public safety sector, not the health sector, all of a sudden saying, ‘We need to address trauma. We need to recognize that when victims go unhelped, it feeds the cycle of crime that we’re trying to stop.’”
When Roberts’s second gunshot wound became the first to land him in an emergency room, he wound up at Cleveland’s MetroHealth Medical Center. Almost as old as the city itself, MetroHealth was founded in 1837 to care for the area’s most vulnerable residents. Today, half of its patients are covered by Medicaid. Until a year and a half ago, it was the only adult Level 1 trauma center in the region. MetroHealth recently became one of two hospitals in Cleveland to join Ohio’s experiment in trauma recovery; the other is University Hospitals, across town. Grants from the state attorney general’s office will equip the hospitals with more resources to support gunshot patients, as well as victims of sexual assault, domestic violence, human trafficking, and hate crimes.
Heather Vallier, an orthopedic trauma surgeon, says that when she started at MetroHealth 17 years ago, it was unusual for her to operate on shooting victims. “Now,” she says, “I’m operating on these people every month.” Vallier only treats a fraction of the total gunshot patients who arrive at MetroHealth’s emergency department, which handled 519 shooting victims in 2016. The number was even higher the year before, when Cleveland was one of 25 major American cities to see its murder rate spike.
Forty percent of MetroHealth’s gunshot patients are treated and released without being admitted, according to Jeff Claridge, a trauma surgeon and director of the trauma division. “We give them a pat on the back, and they get no resources, they get nothing,” he says.

MetroHealth may very well see some of those patients again. In 2013, Claridge co-authored a study that showed that one in four trauma patients returned to the hospital for a separate traumatic injury within five years. Among gunshot and stab wound patients, that rate is even higher, at one in three. Another recent study done at a trauma center in Minneapolis suggests that gunshot victims are susceptible not only to being shot again, but also to sustaining increasingly severe injuries.
John Rich, a public health professor at Drexel University in Philadelphia, puts it this way:
Visiting the hospital for a gunshot injury, he says, opens both a “window of vulnerability, and a window of opportunity.”

For Roberts, the lull between shooting three and shooting four was alarmingly brief. On November 26, 2016, he took a bullet in the leg. The wound was still healing when, eight days later on December 4, he was shot again.
“You’re seeing these folks come in that have been shot three, four, five times by the time they’re 26, 27 years old,” says Sarah Hendrickson, who manages MetroHealth’s survivor recovery services and is overseeing the hospital’s new trauma recovery program. “When you’ve seen the same doctor three times for a gunshot wound, that doctor’s like, ‘Come on, man. What are you doing? What do we do here? How do we help you?’ But… they don’t have a lot of time to sit on that and figure that out.”
Over the past four years, Hendrickson’s small team has been developing methods for supporting trauma patients, like counseling a patient newly paralyzed from a motorcycle accident or matching a fall survivor with a former patient who can relate to the excruciating pain of a pelvic injury. But she says gunshot patients present a particularly tricky group. “We were really disconnected from their needs, and from the barriers many of these individuals faced upon returning to their community.”
For people who walk away from shootings, those needs and those barriers are many and daunting.
Gunshot victims around the country report dealing with chronic pain, post-traumatic stress, lapses in health insurance, housing insecurity, and the high cost of expenses stemming from their injuries. Wayne McNeil of Mobile, Alabama, was gunned down in his front yard in 2012. He told me that he continues to cope with episodes of intense anxiety and panic. Derrick Strong, shot nine times in New Orleans in 2016, is still searching for a physical therapy clinic that will accept his insurance. He’s been without stable housing since the incident, staying with his brother and sister instead.
In Cleveland in March, a safe place to stay was also weighing on the mind of 23-year-old gunshot victim Tyrone Jackson. He’d been living with a girlfriend when he was shot in the finger, foot, and stomach outside a bar. Now he wants to get out of that part of the city.
“I’m really scared for my life,” Jackson said over the phone, laboring to breathe through a tube in his nose in a MetroHealth hospital room. “I don’t know where to even go when I get out of here.”

Ohio’s new trauma recovery network is designed to answer just those sorts of vexing questions. MetroHealth is partnering with the May Dugan Center, a community health and human service nonprofit, to ensure its patients keep getting care. “When you’ve been through a traumatic incident, you’re thinking of a lot of other things besides Googling what resources you need,” says Megen Betts, a recovery coach at the hospital.
Starting in April, a trauma therapist and two newly hired social workers from the community center took up posts in MetroHealth’s emergency department, ready to meet incoming victims of violence and their families and determine what resources they require. In cases like Jackson’s, for instance, patients may be offered a post-discharge hotel stay for up to 15 days. Those 15 days are “inadequate” in regard to a long-term solution, says Sue Marasco, May Dugan’s director of education. But they can give victims a few nights of good rest in a safe place while May Dugan helps them figure out the next step.
The program is still in its early days, but Marasco elaborated on her vision for how it will work:
“Say someone comes in who’s been shot. Their mom, dad, sister, and brother come in right after them. The social worker is going to sit with them and say, ‘I’m so sorry this happened to you. Tell me your story.’ She’ll then say, ‘So what I’m hearing is the son probably should not return to the neighborhood tonight. Second, the son probably won’t want to talk to the police. Third, it’s going to be really hard for this young man to return for the follow-up appointment.’”

Marasco has witnessed what can happen if a patient gets lost in the system. She shared the story of one gunshot victim who, after he didn’t return for a follow-up appointment, had a wound become infected. He ended up going to three different hospitals; at each, he was prescribed a new set of medication. It was only when he came to May Dugan that the center’s nurse noticed he’d been taking a potentially lethal combination of drugs.
The new recovery network hopes to fill those gaps by reaching patients early on. Once patients agree to May Dugan’s help, Marasco’s team will offer to screen them for trauma. After discharge, the patient will be added to the network’s caseload. Team members will call clients once a week for four weeks — arranging counseling sessions, helping them keep track of medication and follow-up appointments, providing transportation and short-term childcare for court hearings.
“We’ll pick them up,” Marasco says. “If they’re not comfortable with that, we can provide bus tickets. If they don’t want to be on the bus with us, we can provide taxis.”
She says that before the trauma recovery network, Cleveland had all the pieces to help crime victims, but they didn’t always sync up. Now, for each obstacle to recovery, May Dugan tries to propose a solution. The safety net that once ended at the hospital’s front door gets extended.
“It’s our job to help them,” Marasco says. “It’s not their job necessarily to reach out to us.”
On a frigid afternoon in March, Matthew Roberts sits in his room at a rehabilitation facility, eyes trained on an NBA video game he’s playing. Tattoos sheathe his neck. An inked dove spreads its wings beneath his ear.
When I visit him, Roberts is weeks away from wrapping up his rehabilitation and returning home. He says he plans to avoid the streets, stop selling drugs, focus on his daughters, get a job — “live my life right.” He now thinks each new bullet that sped through his body was a signal. “Each one was supposed to been a wake-up call, stop doing what I’m doing.”

Victims of street violence often can’t make those kinds of changes alone. If the trauma recovery network works as intended, patients like Roberts will get help they need to steer themselves away from further harm.
“The gunshot alone is not enough of a curveball to throw people off their path,” says Hendrickson, the recovery program’s director. “It’s not the gunshot. It’s all the other circumstances surrounding why they got shot. We need to address those psychosocial factors. I think that’s proper and responsible healthcare.”